Cardiovascular Health Informatics: Wearable Medical Device and Flexible Biosensor for m-Health
By Xiao-Rong Ding, Jing Liu, Ni Zhao, and Yuan-Ting Zhang
Wearable sensors hold the promise of early detection, diagnosis, and treatment of cardiovascular diseases. The key technologies of miniaturization, intelligence, networking, digitalization, and standardization are disussed.
Cardiovascular diseases (CVDs) are the leading cause of death in the world. The death number caused by CVDs, mainly heart disease and stroke, will increase to 23.3 million by 2030 as reported by the World Health Organization [1]. Among all the deaths caused by CVD, about two-thirds of them happen in out-of-hospital settings [2]. In addition, as a result of lacking continuous monitoring and accurate predicting tools, acute cardiovascular events cause a large number of deaths without any prior symptoms or with some symptoms which fail to draw enough attention from the patients [3].
Cardiovascular health informatics is a rapidly evolving interdisciplinary area dealing with the acquisition, transmission, processing, storage, retrieval, interpretation, and use of the information from the cardiovascular system so as to benefit the early detection, early prediction, early prevention, early diagnosis and early treatment of CVDs [4]. With developments in wireless and mobile communication and information technology, mobile health (m-Health), which is referred to mobile computing, medical sensor, and communications technologies for health care [5], is a preferable way both for patients to personalize their healthcare options and adhere to appropriate self-management, and at the same time for professionals to monitor the physiological factors in real time and offer quick responses in case of emergency. Benefiting from the growing advancement of electronics and communication technique, wearable medical devices which can be worn by people and measure physiological parameters like ECG, heart rate (HR), BP, make it possible to monitor the health status continuously or even unobtrusively with an extended period of time. Especially with the development of flexible biosensors which are well conformal to the human body, physiological data can be taken without causing any discomfort to the subjects or influencing their daily activities. Wearable medical device and flexible biosensor can act as excellent terminals in m-Health to interact with the patient to collect the vital signs for remote monitoring and processing center in real time.
In recent years, a variety of unobtrusive wearable medical devices have been developed. Taking the applications of CVDs as an example, there are watch-type BP device, clip-free eyeglasses-based device for measuring heart rate and pulse transit time (PTT), ECG necklace for long-term cardiac activity monitoring, h-Shirt for heart rate and continuous BP measurement, as well as the ring-shape device for heart rate and temperature measurement [6]. Unobtrusive sensing concept with its realization in daily objects developed by our research group is shown in Fig. 1. With the development of wearable technologies, the deployment of the m-Health will be further accelerated in the near future [5].
The key technologies for designing wearable device include Miniaturization, Intelligence, Networking, Digitalization, and Standardization (MINDS) [7]. Through miniaturization, the physical size as well as the power consumption of the device can be essentially reduced, thereby facilitating long-term monitoring and popularizing its use. The intelligence enables automatic diagnosis and alerting. Networking is an essential communication part of wearable device to deliver professional healthcare services with high efficiency and high quality remotely from the standpoint of m-Health. And digitalization is necessary for data analysis and storage after the analog vital signals being acquired in a digital form. Standardization will ensure the performance evaluation and interoperability of the wearable medical device. This paper will focus on an overview of the recent developments of wearable device miniaturization and standardization.
Miniaturization can improve user comfort of the wearable devices, thus better ensuring the long-term and continuous monitoring. Recent technological advances in integrated circuit (IC), new sensing approaches and novel measuring principle have paved the way for the miniaturization of wearable medical devices. Firstly, through integrated circuit (IC) design, the physical size of the wearable device can be largely reduced. The challenges of IC design for wearable devices include power dissipation reduction, and low input-referred noises. These relevant techniques have been reviewed in [8], which could be applied in physiological monitoring to achieve better performance, lower power consumption, and reduced the physical size of the wearable devices. To give an example, a near-infrared HR measurement IC has been designed for processing PPG signal through sheering technique, with cutoff frequency not higher than 0.25Hz and rather low power consumption [9]. A highly integrated microsystem for cardiac vital signs and physical activity monitoring has been implemented by assembling the functional units such as sensor module, signal process, and powering unit into a single platform on a flexible substrate [10].
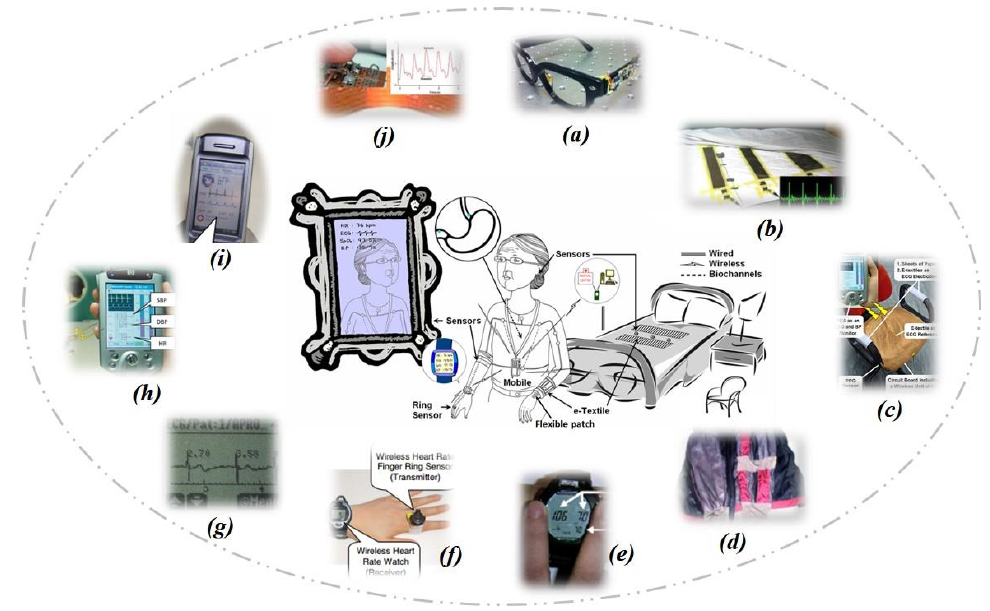
Figure 1: Unobtrusive sensing concept with its realization in daily objects [11]: (a) p-Eyeglasses for physiological monitoring [12]; (b) u-Bed for unobtrusive and continuous monitoring of physiological signals including BP [13]; (c) u-Chair for unobtrusive monitoring of multiple physiological signals [14]; (d) h-Shirt [15]; (e) BP watch [16]; (f) wireless heart rate finger ring sensor [17]; (g) WAP device [18]; (h) PDA-based wireless and cuffless BP meter [19]; (i) mobile-phone-based wireless and cuffless BP meter [17]; and (j) high-sensitivity organic photo-transistor for epidermal and flexible biosensors [20].
Secondly, new sensing approach such as textile-based sensing and epidermal sensing can improve miniaturization due to the development of new material. Textile technology provides a promising approach to integrate various functional modules into a garment, which makes the system lighter and wearable (Fig. 1(d)).Besides, flexible electronics can make wearable sensors conformal to the skin and even can measure the physiological signals unobtrusively. Such devices are referred toepidermal electronic system [21], which upgrade the wearable devices to be thinner, lighter and flexible. There has been increasing interest in flexible biosensor for healthcare application,shown in Figs. 1 and 2. One example is the epidermal electronic system developed by Roger et [22] for measuring electrophysiological signals (ECG and EMG), temperature and strain. The system consists of the multiple sensors, procession units, wireless transmission and powering, which are all mounted on an elastic polymer backing layer. In addition, a flexible capacitive pressure organic thin film transistors with high sensitivity was fabricated by Bao’s team [23], through integrating a microstructured polydimethylsiloxane (PDMS) dielectric with a thin film polymer semiconductor. This device has been applied to measure human radial artery pulse wave with high-fidelity. And very recently, our research group has developed an organic bulk heterojunction based near-infrared photo-transistor which can potentially be used for designing flexible and epidermal devices [20]. The organic transistor shows remarkable performance with responsivity up to 5 x 105 AW-1 as well as wide gain tunability (see Fig. 3). The phototransistor is demonstrated as a detection unit in PPG sensor for continuous measurement of the pulse at the fingertip (Fig. 1(j)). And it can be applied for designing cuffless or even flexible BP device in the near future.
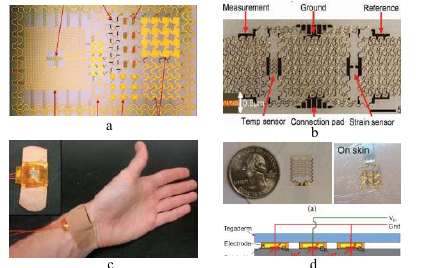
Figure 2: Flexible biosensors for healthcare applications: (a) multifunctional electronics matched to the epidermis [22]; (b) multifunctional epidermal electronic systems [21]; (c) flexible capacitive pressure sensor [23]; and (d) skin sweat patch [24].
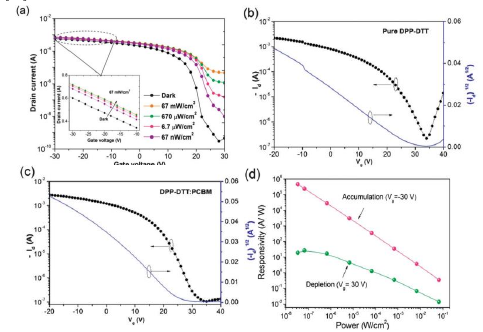
Figure 3: The results of the high-sensitivity organic phototransistor [20], (a) transfer characteristics of the device under dark and illumination condition; and the transfer characteristics in the saturation region of (b) pure DPP-DTT and (c) DPP-DTT: PCBM blends in the dark; and (d) responsivity versus light intensity in the accumulation and depletion regions.
Last but not the least, novel measuring principle through modeling can reform the conventional method, which can contribute to reducing the size of the medical device. The PTT-based BP measurement [25] is a representative example. The current BP devices are usually based on the oscillometric method with an occluding cuff. The cuff not only limits its use for long time monitoring of BP since the process of frequent inflation and deflation will cause discomfort to the subject, but also hinders reducing the size of the device. In the contrast, the cuffless technique, measuring BP through modeling its relationship with other parameters that are measured without any occluding cuff, can be developed into unobtrusive wearable device. Aiming at the cuffless BP measurement and other physiological parameters, we have developed a series of unobtrusive devices, such as the BP device, p-Eyeglasses, u-Bed and u-Chair (Fig. 1).
Standardization is crucial to wearable medical devices as it ensures the objective performance evaluation for their industrialization and facilitates the interoperability and harmonization for their usability in the homecare and the Point of Care Physiological Systems.
Cardiovascular health information involves multiple physiological signals like ECG, BP, and SpO2 in multiple modalities. These parameters may be taken in a completely different way by wearable medical device from the conventional medical devices. Moreover, different wearable medical devices can also take the measurements of the same signal based on different principles. Therefore, a standard for quantitative and objective evaluation of wearable medical device is needed for its industrialization. Taking cuffless BP measuring device as an example, its operation method, error distribution and analysis, result evaluation, and calibration procedure are not totally conformed to the existing standards for sphygmomanometers with an occluding cuff. To assess the accuracy of cuff-less blood pressure measuring, the t4 distribution consistent with experimental data is proposed for evaluating the mean absolute difference (MAD) [26]. In comparison with normal distribution, it does better in depicting the underlying error distribution of wearable BP devices [26]. The result is illustrated in Fig. 4, where the MAD is expressed in terms of mean difference (MD), standard derivation (SD), and v in (1). Adopting this evaluation scale with a single validation criterion of MAD, IEEE P1708 draft standard for wearable cuffless blood pressure measuring devices strengthens the simplicity and comparability between different wearable BP devices for industrialization [27].
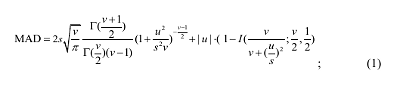
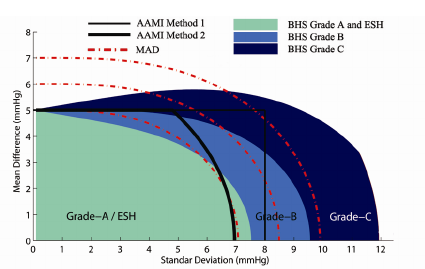
Figure 4: A mapping chart relating MAD with the ANSI/AAMI SP10 and BHS protocol, and ESH criteria [26].
With interoperability by standardization, wearable medical devices of different types, models, or manufacturers are capable of working with each other, whether connected to each other directly or through a communication system. In order to achieve miniaturization, the capabilities of wearable devices are limited to some degree, such as restricted process abilities and storage, small battery, fixed configuration. However, taking advantages of m-Health, the processing and storage task can be transferred from the end device to the external or remote manager by applying the communication standards. ISO/IEEE 11073 Personal Health Device (PHD) is a set of standards that specify nomenclature, domain models, service models, communication models and implementing models for medical device communication, and that aim at “providing real-time plug-and-play interoperability for patient connected medical devices and facilitate the efficient exchange of vital signs and medical device data, acquired at the point-of-care, in all health care environments” [28]. With communication standards for medical device, the format of medical vital signs is well designed and the data flow can properly get though the layers of the architecture of m-health.
In conclusion, with the rapid development in material, sensing, power scavenging and wireless communications, there has been a great increase in the number of new wearable sensing devices for healthcare applications. The further development of unobtrusive wearable devices and flexible biosensors could promote m-Health, which can further advance cardiovascular health informatics through understanding the mechanism of CVDs and preventing the development of CVDs at its early stage, so as to provide a low-cost, efficient and reliable way to realize pervasive healthcare.
Acknowledgement
This work was supported in part by the National Basic Research Program 973 (NO. 2010CB732606), the Guangdong Innovation Research Team Fund for Low-cost Healthcare Technologies in China, the External Cooperation Program of the Chinese Academy of Sciences (NO. GJHZ1212), the Key Lab for Health Informatics of Chinese Academy of Sciences and the National Natural Science Foundation of China (NO. 81101120).
For Further Reading
1. WHO. (2013). Cardiovascular diseases (CVDs). Available: http://www.who.int/mediacentre/factsheets/fs317/en/
2. G. A. Mensah, The atlas of heart disease and stroke: World Health Organization, 2004.
3. M. Naghavi, P. Libby, E. Falk, S. W. Casscells, S. Litovsky, J. Rumberger, et al., “From vulnerable plaque to vulnerable patient a call for new definitions and risk assessment strategies: part I,” Circulation, vol. 108, pp. 1664-1672, 2003.
4. Y. T. Zhang, Y. L. Zheng, W. H. Lin, H. Y. Zhang, and X. L. Zhou, “Challenges and Opportunities in Cardiovascular Health Informatics,” IEEE Transactions on Biomedical Engineering, vol. 60, pp. 633-642, 2013.
5. R. S. Istepanian, E. Jovanov, and Y. Zhang, “Guest editorial introduction to the special section on m-health: Beyond seamless mobility and global wireless health-care connectivity,” Information Technology in Biomedicine, IEEE Transactions on, vol. 8, pp. 405-414, 2004.
6. Y. L. Zheng, X. R. Ding, C. C. Poon, B. Lo, H. Y. Zhang, X. L. Zhou, et al., “Unobtrusive Sensing and Wearable Devices for Health Informatics,” IEEE Transactions on Biomedical Engineering, vol. 0, 2014.
7. C. C. Poon and Y.-T. Zhang, “Perspectives on high technologies for low-cost healthcare,” Engineering in Medicine and Biology Magazine, IEEE, vol. 27, pp. 42-47, 2008.
8. Y. Li, C. C. Poon, and Y.-T. Zhang, “Analog integrated circuits design for processing physiological signals,” Biomedical Engineering, IEEE Reviews in, vol. 3, pp. 93-105, 2010.
9. A. Wong, K.-P. Pun, Y.-T. Zhang, and K. Hung, “A near-infrared heart rate measurement IC with very low cutoff frequency using current steering technique,” Circuits and Systems I: Regular Papers, IEEE Transactions on, vol. 52, pp. 2642-2647, 2005.
10. Y. Chuo, M. Marzencki, B. Hung, C. Jaggernauth, K. Tavakolian, P. Lin, et al., “Mechanically flexible wireless multisensor platform for human physical activity and vitals monitoring,” Biomedical Circuits and Systems, IEEE Transactions on, vol. 4, pp. 281-294, 2010.
11. Y. T. Zhang and C. Poon, “Health Informatics: Unobtrusive Physiological Measurement Technologies,” IEEE Journal of Biomedical and Health Informatics, vol. 17, pp. 893-893, 2013.
12. Y. L. Zheng, B. Leung, S. Sy, Y. T. Zhang, and C. C. Poon, “A clip-free eyeglasses-based wearable monitoring device for measuring photoplethysmograhic signals,” in Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), 2012, pp. 5022-5025.
13. W. Gu, C. Poon, H. Leung, M. Sy, M. Wong, and Y. Zhang, “A novel method for the contactless and continuous measurement of arterial blood pressure on a sleeping bed,” in Annual International Conference of the IEEE in Engineering in Medicine and Biology Society, EMBC. , 2009, pp. 6084-6086.
14. K. F. Wu, C. H. Chan, and Y. T. Zhang, “Contactless and cuffless monitoring of blood pressure on a chair using e-textile materials,” 2006 3rd IEEE/EMBS International Summer School on Medical Devices and Biosensors, pp. 98-100, 2006.
15. W. Gu, C. C. Poon, M. Sy, H. Leung, Y. Liang, and Y. T. Zhang, “A h-shirt-based body sensor network for cuffless calibration and estimation of arterial blood pressure,” in Sixth International Workshop on Wearable and Implantable Body Sensor Networks, BSN, 2009, pp. 151-155.
16. C. C. Poon, Y. M. Wong, and Y.-T. Zhang, “M-health: the development of cuff-less and wearable blood pressure meters for use in body sensor networks,” in IEEE/NLM Life Science Systems and Applications Workshop, 2006, pp. 1-2.
17. Y.-t. Zhang, X. Xiang, and C. C. Poon, “The evaluation of nodes of body sensor networks: wearable blood pressure measuring devices,” in Wearable and Implantable Body Sensor Networks, 2006. BSN 2006. International Workshop on, 2006, pp. 4 pp.-161.
18. K. Hung and Y. Zhang, “WAP-based telemedicine applications,” Australasian Physical & Engineering Science in Medicine, vol. 24, pp. 196-200, 2001.
19. C. C. Poon, Y.-T. Zhang, and S.-D. Bao, “A novel biometrics method to secure wireless body area sensor networks for telemedicine and m-health,” Communications Magazine, IEEE, vol. 44, pp. 73-81, 2006.
20. H. Xu, J. Li, B. H. Leung, C. C. Poon, B. S. Ong, Y. Zhang, et al., “A high-sensitivity near-infrared phototransistor based on an organic bulk heterojunction,” Nanoscale, vol. 5, pp. 11850-5, Dec 7 2013.
21. W. H. Yeo, Y. S. Kim, J. Lee, A. Ameen, L. Shi, M. Li, et al., “Multifunctional epidermal electronics printed directly onto the skin,” Advanced Materials, vol. 25, pp. 2773-2778, 2013.
22. D. H. Kim, N. Lu, R. Ma, Y. S. Kim, R. H. Kim, S. Wang, et al., “Epidermal electronics,” Science, vol. 333, pp. 838-843, 2011.
23. G. Schwartz, B. C. K. Tee, J. Mei, A. L. Appleton, D. H. Kim, H. Wang, et al., “Flexible polymer transistors with high pressure sensitivity for application in electronic skin and health monitoring,” Nature communications, vol. 4, p. 1859, 2013.
24. Y.-Y. Hsu, J. Hoffman, R. Ghaffari, B. Ives, P. Wei, L. Klinker, et al., “Epidermal electronics: Skin sweat patch,” in Microsystems, Packaging, Assembly and Circuits Technology Conference (IMPACT), 2012 7th International, 2012, pp. 228-231.
25. C. Poon and Y. Zhang, “Cuff-less and noninvasive measurements of arterial blood pressure by pulse transit time,” in Engineering in Medicine and Biology Society, 2005. IEEE-EMBS 2005. 27th Annual International Conference of the, 2006, pp. 5877-5880.
26. I. R. Yan, C. C. Y. Poon, and Y.-T. Zhang, “Evaluation scale to assess the accuracy of cuff-less blood pressure measuring devices,” Blood Pressure Monitoring, vol. 14, pp. 257-267, 2009.
27. “IEEE Draft Standard for Wearable Cuffless Blood Pressure Measuring Devices,” IEEE P1708/D03, February 2014, pp. 1-33, 2014.
28. ISO/IEEE, “11073-10101:2004 Health informatics – point-of-care medical device communication Part 10101: nomenclature.,” ed.
Contributors
 Xiao-Rong Ding is currently pursuing her Ph.D. degree in Biomedical Engineering at the Joint Research Centre for Biomedical Engineering of The Chinese University of Hong Kong, Shatin, N.T., Hong Kong. Her research interests include wearable medical devices, CVD health informatics and physiological modelling. Read more
Xiao-Rong Ding is currently pursuing her Ph.D. degree in Biomedical Engineering at the Joint Research Centre for Biomedical Engineering of The Chinese University of Hong Kong, Shatin, N.T., Hong Kong. Her research interests include wearable medical devices, CVD health informatics and physiological modelling. Read more
 Jing Liu is currently working as a short-term research assistant in Joint Research Center for Biomedical Engineering at the Chinese University Hong Kong (CUHK), Shatin, N.T., Hong Kong. Meanwhile, she is a senior student of Wuhan University majoring in Computer Science and she is going to pursue her Ph.D. degree in Biomedical Engineering at CUHK in the autumn of 2014. Her research interests include wearable medical device and physiological modeling. Read more
Jing Liu is currently working as a short-term research assistant in Joint Research Center for Biomedical Engineering at the Chinese University Hong Kong (CUHK), Shatin, N.T., Hong Kong. Meanwhile, she is a senior student of Wuhan University majoring in Computer Science and she is going to pursue her Ph.D. degree in Biomedical Engineering at CUHK in the autumn of 2014. Her research interests include wearable medical device and physiological modeling. Read more
 Ni Zhao is currently an assistant professor at the Department of Electronic Engineering at the Chinese University of Hong Kong, Shatin, N.T., Hong Kong. She received her Ph.D. degree in Physics from the University of Cambridge (UK) in 2008. Her research interest covers optoelectronic, electronic and electrochemical devices based on organic and nanostructured materials; spectroscopic characterization of the physical processes in nanostructured thin films, structures, and devices. Read more
Ni Zhao is currently an assistant professor at the Department of Electronic Engineering at the Chinese University of Hong Kong, Shatin, N.T., Hong Kong. She received her Ph.D. degree in Physics from the University of Cambridge (UK) in 2008. Her research interest covers optoelectronic, electronic and electrochemical devices based on organic and nanostructured materials; spectroscopic characterization of the physical processes in nanostructured thin films, structures, and devices. Read more
 Yuan-Ting Zhang is currently the Director of Joint Research Center for Biomedical Engineering and Professor of Department of Electronic Engineering at the Chinese University of Hong Kong (CUHK), Hong Kong, China. He serves concurrently the Director of the Key Lab for Health Informatics of the Chinese Academy of Sciences (HICAS) at SIAT, Shenzhen, China. He is the founder and the first Director of the SIAT Institute of Biomedical and Health Engineering under the Chinese Academy of Sciences. His research spans several fields including wearable medical devices, flexible biosensors, BSN security, neuro-physiological modeling, CVD health informatics, and m-u-p-Heath technologies. Read more
Yuan-Ting Zhang is currently the Director of Joint Research Center for Biomedical Engineering and Professor of Department of Electronic Engineering at the Chinese University of Hong Kong (CUHK), Hong Kong, China. He serves concurrently the Director of the Key Lab for Health Informatics of the Chinese Academy of Sciences (HICAS) at SIAT, Shenzhen, China. He is the founder and the first Director of the SIAT Institute of Biomedical and Health Engineering under the Chinese Academy of Sciences. His research spans several fields including wearable medical devices, flexible biosensors, BSN security, neuro-physiological modeling, CVD health informatics, and m-u-p-Heath technologies. Read more







 Surapa Thiemjarus is a researcher from the National Electronics and Computer Technology Center (NECTEC), National Science and Technology Development Agency (NSTDA), Thailand. She received her PhD degree in Computing from Imperial College, UK. Her research interests include context-aware and pervasive sensing, body sensor networks and applications, sensor fusion, machine learning, pattern recognition, sound and signal processing, and assistive technologies.
Surapa Thiemjarus is a researcher from the National Electronics and Computer Technology Center (NECTEC), National Science and Technology Development Agency (NSTDA), Thailand. She received her PhD degree in Computing from Imperial College, UK. Her research interests include context-aware and pervasive sensing, body sensor networks and applications, sensor fusion, machine learning, pattern recognition, sound and signal processing, and assistive technologies.  Jing Liu is currently working as a short-term research assistant in Joint Research Center for Biomedical Engineering at the Chinese University Hong Kong (CUHK), Shatin, N.T., Hong Kong. Meanwhile, she is a senior student of Wuhan University majoring in Computer Science and she is going to pursue her Ph.D. degree in Biomedical Engineering at CUHK in the autumn of 2014. Her research interests include wearable medical device and physiological modeling.
Jing Liu is currently working as a short-term research assistant in Joint Research Center for Biomedical Engineering at the Chinese University Hong Kong (CUHK), Shatin, N.T., Hong Kong. Meanwhile, she is a senior student of Wuhan University majoring in Computer Science and she is going to pursue her Ph.D. degree in Biomedical Engineering at CUHK in the autumn of 2014. Her research interests include wearable medical device and physiological modeling.  Xiao-Rong Ding is currently pursuing her Ph.D. degree in Biomedical Engineering at the Joint Research Centre for Biomedical Engineering of The Chinese University of Hong Kong, Shatin, N.T., Hong Kong. Her research interests include wearable medical devices, CVD health informatics and physiological modelling.
Xiao-Rong Ding is currently pursuing her Ph.D. degree in Biomedical Engineering at the Joint Research Centre for Biomedical Engineering of The Chinese University of Hong Kong, Shatin, N.T., Hong Kong. Her research interests include wearable medical devices, CVD health informatics and physiological modelling.  Ni Zhao is currently an assistant professor at the Department of Electronic Engineering at the Chinese University of Hong Kong, Shatin, N.T., Hong Kong. She received her Ph.D. degree in Physics from the University of Cambridge (UK) in 2008. Her research interest covers optoelectronic, electronic and electrochemical devices based on organic and nanostructured materials; spectroscopic characterization of the physical processes in nanostructured thin films, structures, and devices.
Ni Zhao is currently an assistant professor at the Department of Electronic Engineering at the Chinese University of Hong Kong, Shatin, N.T., Hong Kong. She received her Ph.D. degree in Physics from the University of Cambridge (UK) in 2008. Her research interest covers optoelectronic, electronic and electrochemical devices based on organic and nanostructured materials; spectroscopic characterization of the physical processes in nanostructured thin films, structures, and devices.  Yuan-Ting Zhang is currently the Director of Joint Research Center for Biomedical Engineering and Professor of Department of Electronic Engineering at the Chinese University of Hong Kong (CUHK), Hong Kong, China. He serves concurrently the Director of the Key Lab for Health Informatics of the Chinese Academy of Sciences (HICAS) at SIAT, Shenzhen, China. He is the founder and the first Director of the SIAT Institute of Biomedical and Health Engineering under the Chinese Academy of Sciences. His research spans several fields including wearable medical devices, flexible biosensors, BSN security, neuro-physiological modeling, CVD health informatics, and m-u-p-Heath technologies.
Yuan-Ting Zhang is currently the Director of Joint Research Center for Biomedical Engineering and Professor of Department of Electronic Engineering at the Chinese University of Hong Kong (CUHK), Hong Kong, China. He serves concurrently the Director of the Key Lab for Health Informatics of the Chinese Academy of Sciences (HICAS) at SIAT, Shenzhen, China. He is the founder and the first Director of the SIAT Institute of Biomedical and Health Engineering under the Chinese Academy of Sciences. His research spans several fields including wearable medical devices, flexible biosensors, BSN security, neuro-physiological modeling, CVD health informatics, and m-u-p-Heath technologies.  Henry Ip is a post-doctoral research fellow at the Hamlyn Centre, Imperial College London, UK. He is specialised in bio-inspired architectures for low-power Application Specific Integrated Circuits (ASICs), miniature amperometric ASIC arrays for subcellular electrochemical recordings and nano-power continuous-time filters.
Henry Ip is a post-doctoral research fellow at the Hamlyn Centre, Imperial College London, UK. He is specialised in bio-inspired architectures for low-power Application Specific Integrated Circuits (ASICs), miniature amperometric ASIC arrays for subcellular electrochemical recordings and nano-power continuous-time filters.  Guang-Zhong Yang is director and co-founder of the Hamlyn Centre, Imperial College London, UK. Professor Yang's main research interests are in medical imaging, sensing and robotics. He is a Fellow of the Royal Academy of Engineering, fellow of IEEE, IET, AIMBE and a recipient of the Royal Society Research Merit Award and listed in The Times Eureka 'Top 100' in British Science.
Guang-Zhong Yang is director and co-founder of the Hamlyn Centre, Imperial College London, UK. Professor Yang's main research interests are in medical imaging, sensing and robotics. He is a Fellow of the Royal Academy of Engineering, fellow of IEEE, IET, AIMBE and a recipient of the Royal Society Research Merit Award and listed in The Times Eureka 'Top 100' in British Science.