Brain-Computer Interface for Stroke Rehabilitation
By Cuntai Guan, Kai Keng Ang, Christopher Kuah, Effie Chew, Karen Chua
Pilot studies of Brain-computer interface (BCI) rehabilitation, combined with haptic feedback, show significant improvement in patient outcomes.
Worldwide, stroke is one of the leading causes of severe disabilities. Each year, there are around fifteen million new stroke cases across the world. Although more than two third stroke patients get satisfactory recovery after emergency treatment, medication and rehabilitation, the rest of stroke survivors have to undergo a long-term rehabilitation including physio and occupational therapies. For these stroke patients, upper limb weakness and loss of hand function are among the most devastating types of disabilities, which affect their daily lives. Although physiotherapy and occupational therapy are the most common treatments for those patients, the outcome of these treatments is limited by: (i) difficulty in improving the function of the plegic hand, (ii) difficulty in delivering intensive repetitions to patients with plegic hands for neuroplastic change and functional improvements, (iii) lack of motivation to sustain interest in the repetitive exercises, especially when patients go back home, and (iv) lack of immediate biofeedback.
The hypothesis of using BCI for stroke rehabilitation is built upon the following basis: (1) motor imagery activates primary motor cortex and associated brain regions which are responsible for motor planning and motor movement, therefore rehabilitation using motor imagery could lead to motor recovery; (2) BCI provides a contingent feedback for stroke patients so as to reinforce the neural pathway of motor control; (3) real-time feedback to patients provides motivation to patients; (4) mechanical/haptic stimulation (eg. robotics) combined with BCI could provide benefits as tangible feedback.
We conducted three pilot clinical studies involving 66 chronic stroke patients. In these studies, we investigated how BCI was used in conjunction with other devices (robotics, haptic, and transcranial Direct Current Stimulation (tDCS)) to help hemiplegic stroke patients in performing upper limb rehabilitation. The results and observations are summarized as follows:
- We observed statistically and clinically significant outcome improvement in stroke patients, comparing the pre- and post-rehabilitation clinical outcome, measured by Fugl-Meyer Motor Assessment (FMMA) scores;
- In the three-arm clinical study, comprising BCI, haptic and standard human therapist, the BCI group achieved significantly better outcome than the human therapist group.
- fMRI imaging shows statistically significant enhancement in functional connectivity after the rehabilitation;
- Initial indication of structural change might imply possible plasticity effects;
- EEG coherence provides possible prediction for clinical outcome.

Figure 1: A BCI-based Robotic Rehabilitation System for Stroke Patients
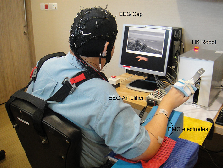
Figure 2: A BCI-based Stroke Rehabilitation System with Haptic Feedback
Figure 1 and 2 show two systems we developed and deployed in the abovementioned clinical studies. Taking the second system (Figure 2) as an example, the system uses BCI to detect the motor intent of hemiplegic patients from the EEG signals to drive a Haptic Knob (HK) with two-degree-of-freedom (i.e. translation and rotation) to train the opening/closing of the hand and pronation/supination of the forearm that excite desired motor cortex with sensory and visual feedback. Its effectiveness and safety were tested through a randomised clinical trial conducted at the Centre for Advanced Rehabilitation Therapeutics (CART) at the Tan Tock Seng Hospital, Singapore. The clinical result of this trial is shown in the table and graph below.
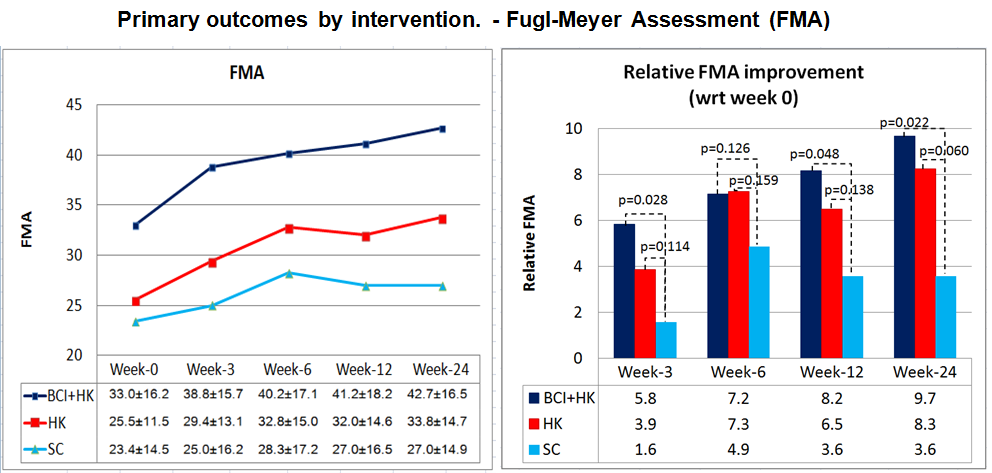
In the trial, patients were randomised into three groups, namely (i) control using Standard Conventional (SC) therapy, (ii) HK robotic only and (iii) BCI+HK. The training intensity is 1 hour 3 times per week for 6 weeks (totally 18 hours). Each group also received an additional 30 minutes of goal-directed therapy addressing functional activities training, tone and postural management. All intervention groups improved and these gains were maintained at week 6, week 12 and week 24. The HK and BCI+HK groups continued to improve even at week 24 when training has ceased for 18 weeks, suggesting that on-going neuroplasticity and/or training effects were operant. At week 24, the FMA gain for the BCI-HK group is significantly higher than the standard therapy group (p=0.022) while the difference between HK and standard therapy group is not statistically significant (p=0.06). This study implies a sustained gain up to 6 month follow-up. It has to be pointed that, the number of subjects in these studies are still relatively small, so it calls for a larger scale clinical trial to validate the efficacy of BCI based stroke rehabilitation.
Acknowledgements:
(1) This work was supported by the Science and Engineering Research Council of A*STAR (Agency for Science, Technology and Research), and the National Medical Research Council, Singapore.
(2) Other contributors: Kok Soon Phua, Chuanchu Wang. Ling Zhao, Wei Peng Teo, Chang Wu Chen, Yee Sien Ng, Longjiang Zhou, Ka Yin Tang, Gopal Joseph Ephraim_Joseph, Haihong Zhang, Zheng Yang Chin, Jeanette Lee, Wilson Low, Beng Ti Ang, Keng-He Kong, Kai Hiang Chuang, Helen Zhou.
For Further Reading
1. K. K. Ang, C. Guan, K. S, Phua, C. Wang, L.Zhou, K. Y. Tang, G. L. Ephraim_Joseph, W. K Kuah, and S. G. Chua, “Brain-Computer Interface-based robotic end effector system for wrist and hand rehabilitation: results of a three-armed randomized controlled trial for chronic stroke”, Frontiers in Neuroengineering, 2014, doi: 10.3389/fneng.2014.00030.
2. K. K. Ang, S. G. Chua, K. S. Phua, C. Wang, Z. Y. Chin, H. Zhang. W. K. Kuah, J. Lee, W. Low, B. T. Ang, K. H. Kong, C. Guan, “A Randomized Controlled Trial on EEG-based motor imagery rain-Computer Interface robotic rehabilitation for stroke”, Clinical EEG & Neuroscience, April, 2014.
3. K. K. Ang, and C. Guan, “-Computer Interface in Stroke Rehabilitation”, Journal of Computer Science and Engineering, vol. 7, no. 2, pp. 139-146, Jun 2013.
4. K. K. Ang, C. Guan, S. G. Chua, B. T. Ang, W. K. Kuah, C.Wang, K. S, Phua, Z. Y. Chin, H. Zhang (2011). “A Large Clinical Study on the Ability of Stroke Patients to Use EEG-Based Motor Imagery Brain-Computer Interface”, Clinical EEG and Neuroscience, vol. 42, no. 4, October 2011, pp. 253-258.
5. B. C. Varkuti, C. Guan, Y. Pan, K. S, Phua, K. K. Ang, W. K. Kuah, S. G.Chua, B. T. Ang, N. Birbaumer, and R. Sitaram (2012). “Resting State Changes in Functional Connectivity Correlate With Movement Recovery for BCI and Robot-Assisted Upper-Extremity Training After Stroke”, Neurorehabilitation & Neural Repair, May 29, 2012, doi:10.1177/1545968312445910
6. J.J. Daly and J. R. Wolpaw (2008).. Brain-computer interfaces in neurological rehabilitation, The Lancet Neurology, vol. 7(11), pp. 1023 – 1043
7. E. Buch, C. Weber, L. G. Cohen, C. Braun, M. A. Dimyan, T. Ard, et al. (2008). “Think to move: a neuromagnetic brain-computer interface (BCI) system for chronic stroke”. Stroke 2008; 39(3): 910-917.
8. J.J. Daly, R. Cheng, J. Rogers, K. Litinas, K. Hrovat, M. Dohring. (2009). “Feasibility of a new application of noninvasive brain computer interface (BCI): a case study of training for recovery of volitional motor control after stroke”. J Neurol Phys Ther 2009; 33(4): 203-211
9. D. Broetz, C. Braun, C. Weber, S. R. Soekadar, A. Caria, N. Birbaumer (2010). “Combination of brain-computer interface training and goal-directed physical therapy in chronic stroke: a case report”. Neurorehab Neural Re 2010; 24(7): 674-679.
10. N. Sharma, V. M. Pomeroy, J-C Baron (2006). “Motor imagery: a backdoor to the motor system after stroke?” Stroke 2006; 37(7): 1941-1952.
11. A. Ramos-Murguialday, D. Broetz, M. Rea, L. Läer, Ö. Yilmaz, F. L. Brasil, et al. (2013).. Brain-machine interface in chronic stroke rehabilitation: a controlled study. Ann. Neurol. 74, 100-108. doi: 10.1002/ana.23879
12. G. Prasad, P. Herman, D. Coyle, S. McDonough, J. Crosbie (2010). “Applying a brain-computer interface to support motor imagery practice in people with stroke for upper limb recovery: a feasibility study”. J Neuroeng Rehabil 2010; 7(1): 60.
13. J. Zhou, J. Yao, J. Deng, J. P. A. Dewald (2009). “EEG-based classification for elbow versus shoulder torque intentions involving stroke subjects”. Comput Biol Med 2009; 39(5): 443-452.
14. K. K. Ang, C. Guan, K. S. Phua, C. Wang, I. The, C. W. Chen, E. Chew (2012). “Transcranial Direct Current Stimulation and EEG-based Motor Imagery BCI for Upper Limb Stroke Rehabilitation”, IEEE Engineering in Medicine and Biology Society (EMBC), Aug 28 – Sept 1, 2012, San Diego, USA, pp 4128-4131.
15.E. Taub, G. Uswatte, M. H. Bowman, V. W. Mark, A. Delgado, C. Bryson, et al.. Constraint-Induced Movement Therapy Combined With Conventional Neurorehabilitation Techniques in Chronic Stroke Patients With Plegic Hands: A Case Series. Arch Phys Med Rehabil. 2013; 94(1): 86-94.
16. T. J. Kimberley, S. Samargia, L. G. Moore, J. K.Shakya, C. E. Lang. Comparison of amounts and types of practice during rehabilitation for traumatic brain injury and stroke. Journal of Rehabilitation Research & Development. 2010; 47(9): 851-61.
17. M. Jurkiewicz, S. Marzolini, P. Oh, Adherence to a Home-Based Exercise Program for Individuals After Stroke. Topics in Stroke Rehabilitation. 2011; 18(3): 277-84.
Contributors
 Dr Cuntai Guan received his Ph.D. degree in Electrical and Electronic Engineering from Southeast University in 1993. He is currently Principal Scientist and Department Head at the Institute for Infocomm Research, Agency for Science, Technology and Research (A*STAR), Singapore. His current research interests include neural and biomedical signal processing; neural and cognitive process and its clinical application; brain-computer interface algorithms, systems and its applications. Read more
Dr Cuntai Guan received his Ph.D. degree in Electrical and Electronic Engineering from Southeast University in 1993. He is currently Principal Scientist and Department Head at the Institute for Infocomm Research, Agency for Science, Technology and Research (A*STAR), Singapore. His current research interests include neural and biomedical signal processing; neural and cognitive process and its clinical application; brain-computer interface algorithms, systems and its applications. Read more
 Dr Kai Keng Ang received his Ph.D. degree in computer engineering from Nanyang Technological University, Singapore. He is currently the Head of Brain-Computer Interface Laboratory and a Scientist with the Institute for Infocomm Research, Agency for Science, Technology and Research, Singapore. His current research interests include brain-computer interfaces, computational intelligence, machine learning, pattern recognition, and signal processing. Read more
Dr Kai Keng Ang received his Ph.D. degree in computer engineering from Nanyang Technological University, Singapore. He is currently the Head of Brain-Computer Interface Laboratory and a Scientist with the Institute for Infocomm Research, Agency for Science, Technology and Research, Singapore. His current research interests include brain-computer interfaces, computational intelligence, machine learning, pattern recognition, and signal processing. Read more
 Mr. Christopher Kuah is a Principal Occupational Therapist currently holding the post of Allied Health Coordinator at the Centre for Advanced Rehabilitation Therapeutics at Tan Tock Seng Hospital. He received his professional qualification in 1995 and attained the Master of Science in Neurorehabilitation from Brunel University (UK) in 2002. His key neurorehabilitation interests include management of clients with hemiplegia and those with complex neuro-disability as a result of stroke and acquired brain injuries. The current focus of his clinical and research work involves development of clinical programs incorporating rehabilitation technologies encompassing robotics, brain-computer interface, and sensor technologies for post-stroke upper limb recovery. Read more
Mr. Christopher Kuah is a Principal Occupational Therapist currently holding the post of Allied Health Coordinator at the Centre for Advanced Rehabilitation Therapeutics at Tan Tock Seng Hospital. He received his professional qualification in 1995 and attained the Master of Science in Neurorehabilitation from Brunel University (UK) in 2002. His key neurorehabilitation interests include management of clients with hemiplegia and those with complex neuro-disability as a result of stroke and acquired brain injuries. The current focus of his clinical and research work involves development of clinical programs incorporating rehabilitation technologies encompassing robotics, brain-computer interface, and sensor technologies for post-stroke upper limb recovery. Read more
 Dr. Effie Chew is Senior Consultant in Rehabilitation Medicine, Division of Neurology, University Medicine Cluster, National University Hospital (NUH), Singapore. She received her MBBS from the University of Melbourne, Australia and her Membership to the Royal College of Physicians (Edinburgh, UK). She completed her Advanced Specialist Training in Rehabilitation Medicine in Singapore and went on to complete a Fellowship in Clinical Neurorehabilitation at Spaulding Rehabilitation Hospital, Harvard Medical School, where she worked in the areas of noninvasive brain stimulation for neuromodulation and neurorecovery, as well as neuropharmacology for cognitive recovery in traumatic brain injury and robotics and motor learning in recovery post-stroke. These continue to be her current areas of research interests. Read more
Dr. Effie Chew is Senior Consultant in Rehabilitation Medicine, Division of Neurology, University Medicine Cluster, National University Hospital (NUH), Singapore. She received her MBBS from the University of Melbourne, Australia and her Membership to the Royal College of Physicians (Edinburgh, UK). She completed her Advanced Specialist Training in Rehabilitation Medicine in Singapore and went on to complete a Fellowship in Clinical Neurorehabilitation at Spaulding Rehabilitation Hospital, Harvard Medical School, where she worked in the areas of noninvasive brain stimulation for neuromodulation and neurorecovery, as well as neuropharmacology for cognitive recovery in traumatic brain injury and robotics and motor learning in recovery post-stroke. These continue to be her current areas of research interests. Read more
 Dr Karen Sui Geok Chua, MBBS (Singapore), FRCP (Edin), FAMS, is currently senior consultant rehabilitation physician practicing at the Tan Tock Seng Hospital Rehabilitation Centre, Singapore. Her special interests include Neurorehabilitation, Spasticity management, including Botulinum toxin therapy, neurolytic blocks and rehabilitation robotics and technology translation. Read more
Dr Karen Sui Geok Chua, MBBS (Singapore), FRCP (Edin), FAMS, is currently senior consultant rehabilitation physician practicing at the Tan Tock Seng Hospital Rehabilitation Centre, Singapore. Her special interests include Neurorehabilitation, Spasticity management, including Botulinum toxin therapy, neurolytic blocks and rehabilitation robotics and technology translation. Read more







 Nitish V. Thakor (F'1994) is a Professor of Biomedical Engineering at Johns Hopkins University, Provost Chair Professor at National University of Singapore, and also the Director of the Singapore Institute for Neurotechnology (SINAPSE) at the National University of Singapore. His expertise is in the field of Neurotechnology and Medical Instrumentation.
Nitish V. Thakor (F'1994) is a Professor of Biomedical Engineering at Johns Hopkins University, Provost Chair Professor at National University of Singapore, and also the Director of the Singapore Institute for Neurotechnology (SINAPSE) at the National University of Singapore. His expertise is in the field of Neurotechnology and Medical Instrumentation.  Nigel Lovell is Scientia Professor at the Graduate School of Biomedical Engineering, University of New South Wales (UNSW), Sydney, Australia.
Nigel Lovell is Scientia Professor at the Graduate School of Biomedical Engineering, University of New South Wales (UNSW), Sydney, Australia.  José del R. Millán the Defitech Professor at the Ecole Polytechnique Fédérale de Lausanne (EPFL) where he explores the use of brain signals for multimodal interaction and, in particular, the development of non-invasive brain-controlled robots and neuroprostheses. In this multidisciplinary research effort, Dr. Millán is bringing together his pioneering work on the two fields of brain-machine interfaces and adaptive intelligent robotics. He received his Ph.D. in computer science from the Univ. Politècnica de Catalunya (Barcelona, Spain) in 1992.
José del R. Millán the Defitech Professor at the Ecole Polytechnique Fédérale de Lausanne (EPFL) where he explores the use of brain signals for multimodal interaction and, in particular, the development of non-invasive brain-controlled robots and neuroprostheses. In this multidisciplinary research effort, Dr. Millán is bringing together his pioneering work on the two fields of brain-machine interfaces and adaptive intelligent robotics. He received his Ph.D. in computer science from the Univ. Politècnica de Catalunya (Barcelona, Spain) in 1992.  Dr Cuntai Guan received his Ph.D. degree in Electrical and Electronic Engineering from Southeast University in 1993. He is currently Principal Scientist and Department Head at the Institute for Infocomm Research, Agency for Science, Technology and Research (A*STAR), Singapore. His current research interests include neural and biomedical signal processing; neural and cognitive process and its clinical application; brain-computer interface algorithms, systems and its applications.
Dr Cuntai Guan received his Ph.D. degree in Electrical and Electronic Engineering from Southeast University in 1993. He is currently Principal Scientist and Department Head at the Institute for Infocomm Research, Agency for Science, Technology and Research (A*STAR), Singapore. His current research interests include neural and biomedical signal processing; neural and cognitive process and its clinical application; brain-computer interface algorithms, systems and its applications.  Dr Kai Keng Ang received his Ph.D. degree in computer engineering from Nanyang Technological University, Singapore. He is currently the Head of Brain-Computer Interface Laboratory and a Scientist with the Institute for Infocomm Research, Agency for Science, Technology and Research, Singapore. His current research interests include brain-computer interfaces, computational intelligence, machine learning, pattern recognition, and signal processing.
Dr Kai Keng Ang received his Ph.D. degree in computer engineering from Nanyang Technological University, Singapore. He is currently the Head of Brain-Computer Interface Laboratory and a Scientist with the Institute for Infocomm Research, Agency for Science, Technology and Research, Singapore. His current research interests include brain-computer interfaces, computational intelligence, machine learning, pattern recognition, and signal processing.  Mr. Christopher Kuah is a Principal Occupational Therapist currently holding the post of Allied Health Coordinator at the Centre for Advanced Rehabilitation Therapeutics at Tan Tock Seng Hospital. He received his professional qualification in 1995 and attained the Master of Science in Neurorehabilitation from Brunel University (UK) in 2002. His key neurorehabilitation interests include management of clients with hemiplegia and those with complex neuro-disability as a result of stroke and acquired brain injuries. The current focus of his clinical and research work involves development of clinical programs incorporating rehabilitation technologies encompassing robotics, brain-computer interface, and sensor technologies for post-stroke upper limb recovery.
Mr. Christopher Kuah is a Principal Occupational Therapist currently holding the post of Allied Health Coordinator at the Centre for Advanced Rehabilitation Therapeutics at Tan Tock Seng Hospital. He received his professional qualification in 1995 and attained the Master of Science in Neurorehabilitation from Brunel University (UK) in 2002. His key neurorehabilitation interests include management of clients with hemiplegia and those with complex neuro-disability as a result of stroke and acquired brain injuries. The current focus of his clinical and research work involves development of clinical programs incorporating rehabilitation technologies encompassing robotics, brain-computer interface, and sensor technologies for post-stroke upper limb recovery.  Dr Karen Sui Geok Chua, MBBS (Singapore), FRCP (Edin), FAMS, is currently senior consultant rehabilitation physician practicing at the Tan Tock Seng Hospital Rehabilitation Centre, Singapore. Her special interests include Neurorehabilitation, Spasticity management, including Botulinum toxin therapy, neurolytic blocks and rehabilitation robotics and technology translation.
Dr Karen Sui Geok Chua, MBBS (Singapore), FRCP (Edin), FAMS, is currently senior consultant rehabilitation physician practicing at the Tan Tock Seng Hospital Rehabilitation Centre, Singapore. Her special interests include Neurorehabilitation, Spasticity management, including Botulinum toxin therapy, neurolytic blocks and rehabilitation robotics and technology translation.