The Global Need for Distributed Healthcare
By Olaf Such
Globally, we face a crisis as countries attempt to deal with a continually increasing need for healthcare. A change to a distributed healthcare system can address this problem.
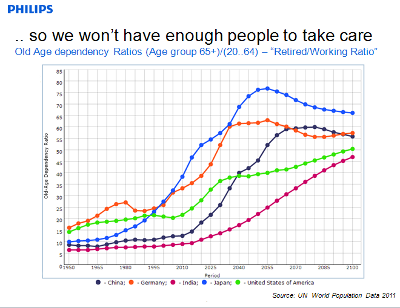
Global demographics show alarming indicators that will affect the capability to provide healthcare within the next generation. OECD and UN data predicts a massive growth in the population over 65, and a parallel decline in the age group between 20 and 65. We observe rising chronic disease prevalence, and less available care capacity to deal with these as a result. This trend is universal, but happening in different rates and timelines across the globe. The current delivery model that has emerged in mature geographies will not be sustainable in this context, for at least three reasons.
The reason usually mentioned first is economic – the cost of care is rising to levels that are arguably not sustainable. The US spent 17,5% of GDP on Healthcare in 2010, and growing. This pattern is seen across all mature economies. This rising cost of healthcare needs to be paid by the productive working population that drives the various economies, which leads to the second reason, which is less often mentioned: There will simply not be enough trained personnel to perform the care tasks in the current model. 2020 predictions are estimating a nurse shortfall of close to 1 million in the US alone. Even if the cost can be paid, it is completely unclear where this workforce will be sourced from, how they will be trained, motivated and kept productive over a lifelong employment. The current model of nurse immigration that is seen in many countries is a local response, but globally unsustainable as demand will increase also in the emigrants’ home countries. Hence, the third reason that this model will not hold further is the strain that this care model puts on caregivers – healthcare professionals, like nurses, and even more so, the informal caregivers in close contact with a patient. Increasingly, caregivers are suffering from collateral diseases, leading to widespread depression, burn out, and other socio-economically devastating consequences.
From a control theory perspective, the feedback loops that are in place in the current system have lead to an optimization towards an inefficient and ineffective system. The care model deployed today has been designed around a reactive “break-fix” concept of centralized care. Centers of excellence are in place to treat acute diseases and are becoming highly specialized in doing so. The technology analogy that can be used here is the one of the mainframe computer, or centralized telephony. This model has its roots in providing care for acute disease, and monetary incentives, as well as efficiency drivers, have lead to growth in this model, which is highly geared towards a medical “repair” shop approach that works for acute disease. However, it can be predicted that it will not sustain for the growing needs of preventative and chronic care.
A paradigm that has the promise to break up this dilemma is “Distributed Healthcare”. By taking a patient centric view on personal care needs, and designing a care model around the needs, and the associated data flow that is derived from the medical decision making following this care cycle, the current centralized model of “break-fix” care delivery can be complemented by a more effective, efficient, and patient friendly approach that has promise to deliver on primary and secondary prevention. This innovation trajectory will be fueled by technology advancements, clinical evidence creation, and socioeconomic modeling. There are already initial examples of these approaches emerging on the markets, and the slow adoption of these models has given these bad press by technology-minded analysts. However, this is not unexpected. Analysis based on Rogers theory of innovation diffusion showed that healthcare innovation takes an average of 17 years from first proof in clinical practice to broad adoption.
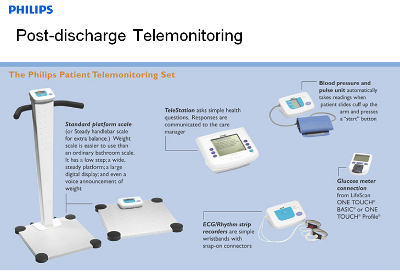
From a technology perspective, the predictions on distributed healthcare are relatively straightforward: Building on Information Technology, MobileWireless platforms and universal network coverage, the devices and solutions that will support the distributed care model will follow trends we have seen in mobile telephony, office automation, and video/data transmission. Systems currently used in a mainframe context needing expert users to interpret data will diverge into subfunctions of information collection, and data interpretation, allowing to unlock the current 1:1 caregiver/patient relationship in time and space. Data can be collected remotely, analyzed centrally, and interventions prescribed again in a distributed fashion. Initial remote patient care examples, like Philips Motiva, Post Discharge Telemonitoring, and initiatives like Continua Health Alliance (http://www.continuaalliance.org) are indicators of this trend that has the promise to provide affordable, accessible care to a rising global patient population in a sustainable way.







 Olaf Such is currently the Global Head of Clinical Science, Magnetic Resonance Imaging Systems, Philips Healthcare, based in Best, the Netherlands.
Olaf Such is currently the Global Head of Clinical Science, Magnetic Resonance Imaging Systems, Philips Healthcare, based in Best, the Netherlands.  Atam P. Dhawan, Ph.D., obtained his bachelor's and master's degrees from the Indian Institute of Technology, Roorkee, and Ph.D. from the University of Manitoba, in Electrical Engineering.
Atam P. Dhawan, Ph.D., obtained his bachelor's and master's degrees from the Indian Institute of Technology, Roorkee, and Ph.D. from the University of Manitoba, in Electrical Engineering.  Mary Capelli-Schellpfeffer, MD, MPA, is Medical Director of Loyola University Health System's Occupational Health Services, and Associate Professor, Department of Medicine...
Mary Capelli-Schellpfeffer, MD, MPA, is Medical Director of Loyola University Health System's Occupational Health Services, and Associate Professor, Department of Medicine...