Body area sensor networks: Requirements, operations, and challenges
By Blessy Johny and Alagan Anpalagan
NOTE: This is an overview of the entire article, which appeared in the March/April 2014 issue of IEEE Potentials magazine.
Click here to read the entire article.
Click here to access the March/April 2014 issue of IEEE Potentials magazine.
Body area networks (BANs) can tackle health care monitoring and delivery challenges through wireless technology and mobile and cloud computing using independent sensors and actuators attached to the body.
In a wireless BAN, the nodes or sensors are placed on the body or on everyday clothing. Several of these sensors are connected to a central processor, which transfers the data to a medical network where health care professionals assess the user’s health condition. A key attribute of a BAN is that it allows medical data to be sampled, processed, and transmitted while the user is at home or on the move.
BANS can bring about radical changes in the health care delivered by ambulances, emergency rooms, operation theaters, clinics, and homes. It aims at detecting any short-or long-term abnormalities in users, the regulation of treatment procedures, alerting the caregiver in case of an emergency, and improving patient comfort.
Biomedical sensors are interconnected into a system to form a body area sensor network (BASN). The term BASN is used when referring to telemedicine or m-health that involves mobile communication, networking, and computing. A BASN node acts as an interface, helping in processing and transmitting data in medical applications.
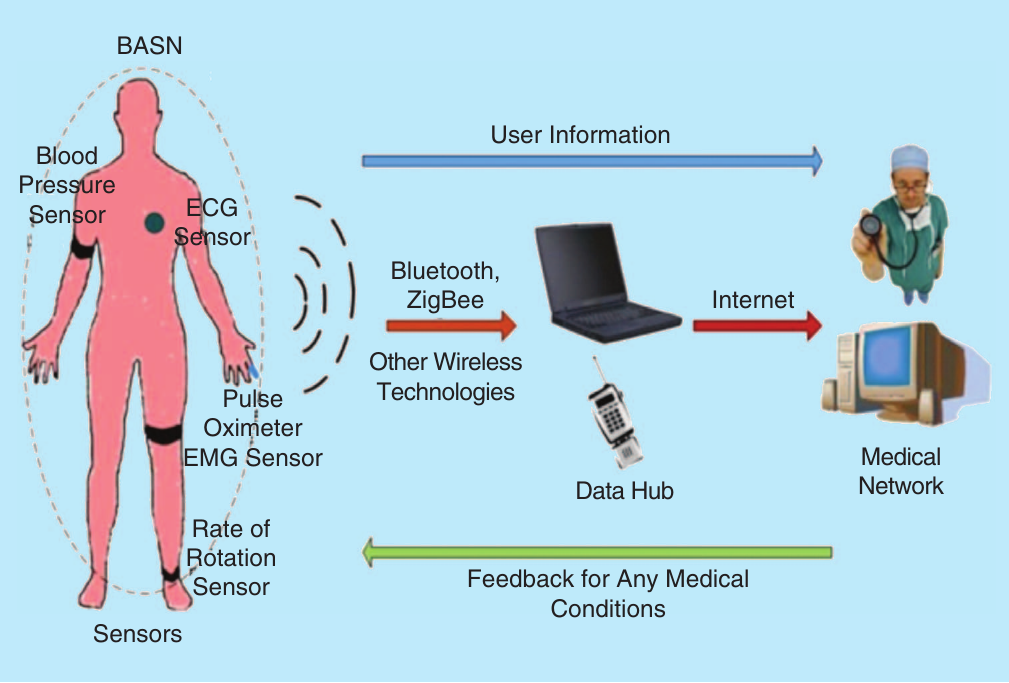
The architecture of a body area sensor network.
BASNs employ a three-tiered architectural system that is designed to meet technical specifications for its optimal and efficient operation. These include the sensors, the data hub, and the medical network, each stage having a unique location and function. The sensors receive signals from the body and relay them to the data hub (usually a cellphone or PDA), which stores for immediate or later releaseto a medical network.
There are three different kinds of sensors. Physiological sensors are used to measure parameters such as blood pressure; blood glucose level; temperature; blood oxygen level; and the signals related to ECG, EEG, and EMG. Biokinetic sensors are used to measure the acceleration and the angular rate of rotation that results from body movements. Ambient sensors are used to measure environmental factors such as temperature, humidity, light, and the sound pressure level.
The medical network is the most crucial tier as it receives all the information about the patient’s medical status, which is then assessed by physicians. The medical network is usually operated by a hospital, clinic, or a telemedicine center. The network has to protect all personal data and handle multiple users. If a threatening medical condition is detected, biofeedback systems can be astivated within a BASN. These systems can trigger a treatment procedure when a medical condition is detected in the user. For example, if the blood glucose level is low or high, an implanted sensor detects the level of sugar and wirelessly triggers an insulin pump to regulate the amount to be injected.
The article discusses the very important consideration of energy consumption (battery life is often a limiting factor in BASNs). Challenges and directions for future research are covered in the full article.
ABOUT THE AUTHORS
Blessy Johny (blessy.johny@ryerson.ca) is a final-year B.Eng. student in biomedical engineering at Ryerson University, Toronto, Canada. In 2013, she worked as a Ryerson research assistant in WINCORE Lab at Ryerson University.
Alagan Anpalagan (alagan@ee.ryerson.ca) is a professor and director in WINCORE Lab in the Department of Electrical and Computer Engineering at Ryerson University, Toronto, Canada. He holds a Ph.D. in wireless communications and networking from the University of Toronto. He is a coauthor of Design and Deployment of Small Cell Networks, Routing in Opportunistic Networks, and Handbook on Green Information and Communication Systems.






